Epidemiology & Disease Burden
- Most common cause of acquired, nonatherosclerotic heart disease worldwide.
- Global prevalence estimated at 33.4 million in 2015, rising to 40.5 million in 2019.
- Approximately 300,000 deaths annually worldwide.
- Predominantly afflicts disadvantaged, marginalized populations in low- and middle-income (LMI) countries (Sub-Saharan Africa, South Asia, Oceania).
- Acute Rheumatic Fever (ARF) peaks between 5-14 years of age.
- RHD prevalence peaks in adulthood between 20-44 years.
- Female predominance, especially after age 15.
Etiopathogenesis
- Immunological disorder initiated by Group A beta-hemolytic streptococci (GAS) pharyngitis.
- Latent period of 10 days to several weeks between pharyngitis and ARF onset.
Molecular Mimicry Mechanism
| Feature | Description |
|---|---|
| Concept | Host and micro-organism share T-cell epitopes. |
| Antigens | GAS M protein and carbohydrate antigen (-acetyl--D-glucosamine). |
| Host Targets | Human cardiac myosin and laminin on heart valves. |
| Immune Response | T-cell activation (CD4+). B-cell antibody production (IgM, IgG). |
| Endocardial Injury | Humoral immune response damages endothelium. Expression of vascular cell adhesion molecule 1 (VCAM-1). CD4+, CD8+, and macrophages infiltrate connective tissue core. Neovascularization occurs. |
Genetic Predisposition
- Monozygotic twin susceptibility significantly higher than dizygotic twins.
- Polymorphisms in candidate genes controlling inflammatory mediators (TGFB1, IL1B, IL10, TNF, CTLA4) associated with RHD susceptibility.
Diagnostic Criteria: Revised Jones Criteria (2015)
- Requires evidence of preceding GAS infection + 2 Major criteria OR 1 Major + 2 Minor criteria.
- For ARF recurrences: 3 Minor criteria sufficient.
Population Definition
Low-Risk Populations
- Acute rheumatic fever incidence <2 per 100,000 school-going children.
- Rheumatic heart disease (RHD) prevalence <1 per 1,000 population.
Moderate and High-Risk Populations
- Rheumatic heart disease (RHD) prevalence ≥ 1 per 1,000 population.
- Applies to populations not strictly meeting low-risk epidemiological thresholds.
Essential Criteria
- Positive throat culture or rapid streptococcal antigen test.
- Elevated or rising anti-streptococcal antibody titer (e.g., ASO titer >250 units, Anti-DNase B).
- Recent scarlet fever.
Major and Minor Criteria (Stratified by Risk)
| Criteria Category | Low-Risk Populations | Moderate/High-Risk Populations |
|---|---|---|
| Major | - Carditis (clinical/subclinical) - Polyarthritis - Chorea - Erythema marginatum - Subcutaneous nodules | - Carditis (clinical/subclinical) - Monoarthritis, Polyarthritis, Polyarthralgia - Chorea - Erythema marginatum - Subcutaneous nodules |
| Minor | - Polyarthralgia or Monoarthritis - Fever ( 38.5°C) - ESR 60 mm/hr OR CRP 3.0 mg/dL - Prolonged PR interval | - Monoarthralgia - Fever ( 38.0°C) - ESR 30 mm/hr OR CRP 3.0 mg/dL - Prolonged PR interval |
Clinical Manifestations
Non-Cardiac Manifestations
- Arthritis: Earliest manifestation (60-80% cases). Migratory polyarthritis involving large joints (knees, ankles, elbows). Swelling, warmth, redness, severe pain. Leaves no residual damage.
- Sydenham’s Chorea: Late manifestation (1-6 months post-infection). Semi-purposeful, jerky, involuntary movements. Emotional lability. Self-limiting course of 2-6 weeks.
- Subcutaneous Nodules: Late manifestation. Painless, firm nodules over bony prominences (elbows, shins, occiput). Highly associated with severe carditis.
- Erythema Marginatum: Early, rare. Faintly reddish, non-itching, serpiginous rash with pale centers. Predominantly on trunk.
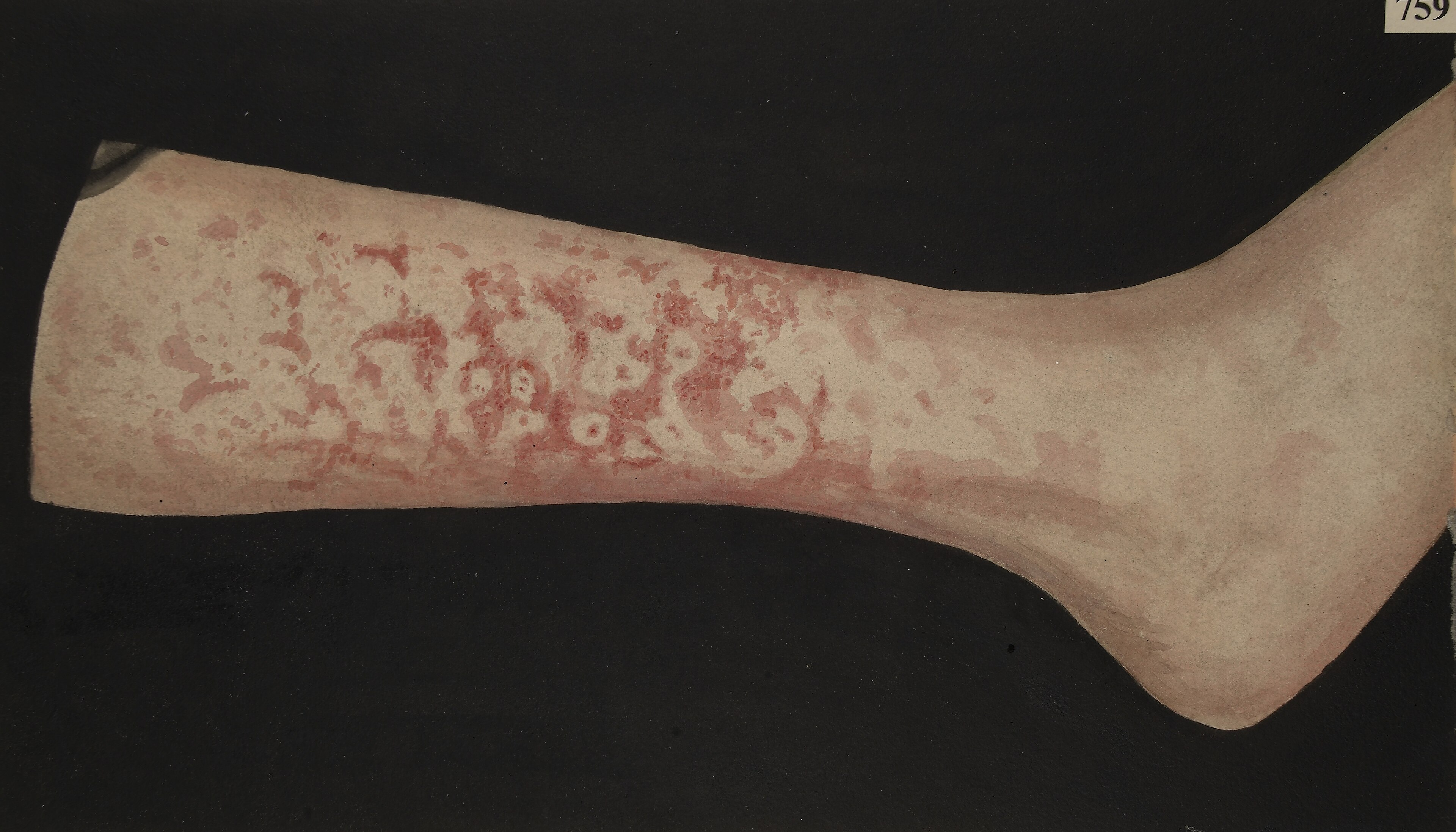 Erythema Marginatum
Erythema Marginatum
Cardiac Manifestations (Carditis & Chronic RHD)
- Pancarditis involving pericardium, myocardium, and endocardium. Valvular damage permanent.
- Subclinical Carditis: Silent clinically. Identified exclusively via echocardiography demonstrating pathological regurgitation.
Mitral Regurgitation (MR)
- Commonest manifestation of acute and chronic rheumatic carditis.
- Pathophysiology: Annular dilatation, chordal elongation/rupture causing anterior leaflet prolapse, focal nodular leaflet thickening. Left atrial and ventricular volume overload.
- Hemodynamics: Systolic leak into left atrium. Rapid filling in early diastole causes third heart sound (S3). Increased left atrial pressure leads to pulmonary congestion.
- Clinical Signs: Displaced, hyperkinetic apex. Pansystolic murmur best heard at apex, radiating to axilla. Wide split S2. Carey Coombs murmur (soft delayed diastolic murmur) in acute phase.
Mitral Stenosis (MS)
- Chronic process requiring 10 years to establish. Result of fibrosis, commissural adhesions, and contracture of leaflets/chordae.
- Pathophysiology: Restricted leaflet motion. Impaired left ventricular filling. Left atrial hypertrophy, pulmonary venous hypertension, elevated pulmonary vascular resistance, right ventricular failure.
- Clinical Signs: Dyspnea, cough, hemoptysis, paroxysmal nocturnal dyspnea. Tapping apex. Loud S1. Opening snap. Mid-diastolic rumbling murmur with presystolic accentuation.
Aortic Regurgitation (AR)
- Isolated pure rheumatic AR extremely rare; almost always accompanies mitral disease.
- Pathophysiology: Sclerosis, distortion, and retraction of cusps. Left ventricular volume overload, dilatation, and hypertrophy.
- Clinical Signs: Wide pulse pressure. Early diastolic decrescendo murmur at left sternal border.
Tricuspid Regurgitation (TR)
- Primary involvement rare. Usually functional secondary to left-sided valvular disease, right ventricular dilatation, and pulmonary hypertension.
- Clinical Signs: Prominent jugular V waves. Systolic hepatic pulsations. Holosystolic murmur at lower left sternal border, increasing with inspiration.
Investigations
Echocardiography (Gold Standard)
- Excludes subclinical carditis. Mandated in modern Jones Criteria.
- Acute Changes: Annular dilation, chordal elongation, flail leaflet, anterior leaflet tip prolapse, beading/nodularity of leaflet tips.
- Chronic Changes: Leaflet thickening, chordal thickening/fusion, restricted leaflet motion, calcification.
- MS Specifics: “Hockey-stick” appearance of anterior mitral leaflet in diastole.
- Color Doppler: Quantifies severity of regurgitant jets (jet length, peak velocity, pan-systolic/pan-diastolic nature).
Electrocardiography (ECG)
- Prolonged PR interval (non-specific, does not alone indicate carditis).
- Advanced AV block (rare).
- P-mitrale (broad, bifid P waves) indicating left atrial enlargement.
- RV/LV hypertrophy signs depending on specific valvular lesion.
- Atrial fibrillation common in advanced chronic MS.
Radiography (CXR)
- Cardiomegaly (left atrial/ventricular enlargement).
- Pulmonary venous congestion, prominent hilar vessels.
- Kerley B lines in advanced MS.
- Double atrial shadow, elevation of left bronchus in massive LA enlargement.
Laboratory Evaluation
- Acute Phase Reactants: Elevated ESR and CRP. Normalize with steroid therapy or resolution of active inflammation.
- Streptococcal Antibodies: ASO titer (>250 units suggestive of recent infection). Anti-DNase B.
Management Strategies
Medical Management of Acute Rheumatic Fever
- Eradication of GAS: Single intramuscular injection of Benzathine Penicillin G. Alternatives: Oral Penicillin V for 10 days, or Azithromycin (if penicillin allergic).
- Anti-inflammatory Therapy:
- Arthritis/Mild Carditis: High-dose Aspirin or NSAIDs (Naproxen).
- Severe Carditis (with CHF): Corticosteroids (Prednisone/Methylprednisolone) indicated to rapidly suppress inflammation, resolve friction rubs, and manage severe hemodynamic compromise.
- Heart Failure Management:
- Diuretics (Furosemide) for volume overload.
- ACE inhibitors or Angiotensin Receptor Blockers (ARBs) for afterload reduction in severe regurgitation.
- Beta-blockers (Carvedilol). Digoxin in select cases. Caution with vasodilators to avoid hypotension.
Secondary Prophylaxis
- Crucial to prevent recurrent ARF and progressive valvular damage.
- Regimen: Intramuscular Benzathine Penicillin G every 3 to 4 weeks. (Every 2 weeks in highly endemic regions for patients <30 kg).
- Duration (AHA Guidelines):
| Patient Category | Recommended Duration |
|---|---|
| ARF without carditis | 5 years after last ARF episode OR until age 21 (whichever is longer). |
| ARF with carditis, NO residual RHD | 10 years after last ARF episode OR until age 21 (whichever is longer). |
| ARF with carditis AND residual RHD | 10 years after last ARF episode OR until age 40 (whichever is longer). Lifelong prophylaxis often required. |
Surgical & Interventional Management
- Indicated for refractory heart failure, severe symptoms despite medical therapy, or progressive cardiomegaly.
- Mitral Valve Repair: Preferred over replacement in children/adolescents. Involves annuloplasty, chordal reconstruction. Avoids need for lifelong anticoagulation.
- Mitral Valve Replacement: Indicated when repair unfeasible. Requires lifelong anticoagulation (Warfarin) with strict INR monitoring. High risk of mechanical valve thrombosis or structural failure of bioprosthetic valves in young patients.
- Percutaneous Balloon Mitral Valvotomy: Treatment of choice for rheumatic MS without severe calcification, marked subvalvular fusion, or significant concomitant MR.
- Aortic Valve Surgery: Repair rarely feasible. Replacement via mechanical prosthesis or homograft.
Complications & Prognosis
Short-Term & Long-Term Complications
- Congestive Heart Failure: Primary cause of morbidity and mortality.
- Arrhythmias: Atrial fibrillation (AF) strongly associated with left atrial dilation in MS. High risk of thromboembolism.
- Thromboembolism: Systemic embolization leading to stroke. Incidence elevated in AF and massive left atrial enlargement.
- Infective Endocarditis: Damaged endothelium serves as nidus. Risk mandates rigorous dental hygiene. Antibiotic prophylaxis indicated prior to bacteremia-inducing procedures in patients with established RHD or prosthetic valves.
- Pulmonary Hypertension: Irreversible pulmonary vascular disease consequence of untreated, long-standing left-sided valvular lesions.
Prognosis
- Determined by severity of initial carditis and frequency of recurrent ARF episodes.
- Post-ARF progression to RHD occurs in ~60-65% of patients.
- Timely secondary prophylaxis drastically reduces morbidity. Non-compliance results in progressive valvular destruction, heart failure, and premature mortality often in the 3rd or 4th decade of life.
